|
ĭespite their discovery in 1900, the critical role of ABO blood groups in transfusion medicine, and their apparent link to multiple diseases, the association of blood groups with mortality in the general population has not been evaluated in a large prospective study. Some of the most consistent associations observed so far include the associations between non-O blood groups and pancreatic cancer (which was also confirmed in a genome-wide association study (GWAS) ), and between the A blood group and gastric cancer and atrophic gastritis. ABO blood groups have also been extensively studied in association with cancer. Higher levels of factor VIII and vWF lead to increased thrombotic tendency, and plasma cholesterol is a known risk factor for atherosclerosis. This association is thought to be mainly due to the higher level of factor VIII and vWF in these individuals, and to some extent the association of blood group locus variants with plasma lipid levels, especially cholesterol. Many vascular disorders (especially venous thromboembolism and atherosclerotic disease) have been linked to non-O blood group status. So, it is not surprising that it has been studied in the context of many chronic diseases. The ABO(H) blood group system was the first genetic polymorphism discovered in humans. However, the only documented roles, so far, include susceptibility to certain infections such as Plasmodium falciparum and Helicobacter pylori, and the level and structure of the von Willebrand Factor (vWF)-FVIII complex in blood. Although blood group antigens have been widely recognized because of the complications they produce in transfusion medicine, their conservation through evolution and their presence on many cells in the human body suggest they are also critical to human physiology. Ford, the renowned geneticist, was quoted in 1945 as saying, ‘It is reasonable to conclude, from what we know of polymorphisms, that individuals belonging to the different blood groups are not equally viable…’. Non-O blood groups have an increased mortality, particularly due to cardiovascular diseases, which may be due to the effect of blood group alleles on blood biochemistry or their effect on von Willebrand factor and factor VIII levels.Į.B. In a subgroup of cohort participants, we also showed higher plasma total cholesterol and low-density lipoprotein (LDL) in those with blood group A. Blood group was not significantly associated with overall cancer mortality, but people with group A, group B, and all non-O blood groups combined had increased risk of incident gastric cancer. Non-O blood groups were associated with significantly increased total mortality (hazard ratio (HR) = 1.09 95% confidence interval (CI): 1.01 to 1.17) and cardiovascular disease mortality (HR = 1.15 95% CI: 1.03 to 1.27). Resultsĭuring a total of 346,708 person-years of follow-up (mean duration 6.9 years), 3,623 cohort participants died. We used Cox regression models adjusted for age, sex, smoking, socioeconomic status, ethnicity, place of residence, education and opium use. In this cohort, 50,045 people 40- to 70-years old were recruited between 20, and followed annually to capture all incident cancers and deaths due to any cause. We aimed to study the association between ABO blood groups and overall and cause-specific mortality in the Golestan Cohort Study. No large population-based study has explored this association with overall and cause-specific mortality. If you have blood type O (phenotype) this means that you inherited neither the allele for antigen ‘A’ nor that for antigen ‘B’.A few studies have shown an association between blood group alleles and vascular disease, including atherosclerosis, which is thought to be due to the higher level of von Willebrand factor in these individuals and the association of blood group locus variants with plasma lipid levels. Our blood type is determined by a paired gene that we receive from our parents – an allele from each parent. Donors with type O+ are allowed to donate to all other Rh+ blood types. Hence, O+ patients are allowed to receive blood only from type O donors (O+ or O-) given all other pre-transfusion tests have been cleared. Donor blood that contains A and/or B antigens will lead to complications and may even result in the death of an O+ recipient. 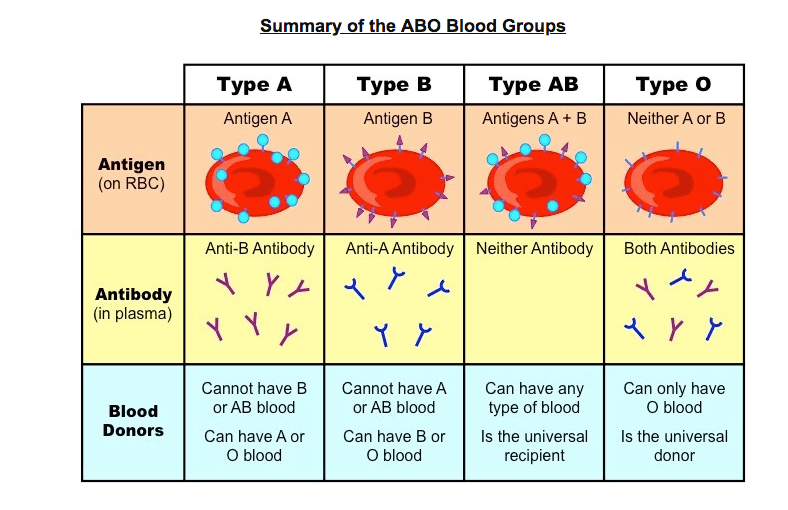
This is because these two antigens are foreign to your body. If you are blood type O+, then you will produce antibodies against A and B antigens. O+Ĭlose to 36.4% of the world’s population has blood type O+. 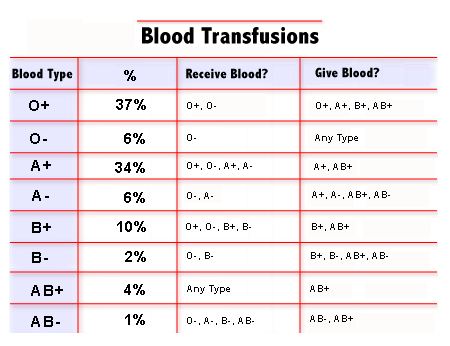
The presence or absence of the Rh factor is denoted by a ‘+’ or ‘-’ behind the blood type, e.g. 
Rhesus-positive (Rh+) people have the Rh factor present while Rhesus-negative (Rh-) do not have the Rh factor. The Rhesus factor is another set of antigens present or absent on RBC.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
